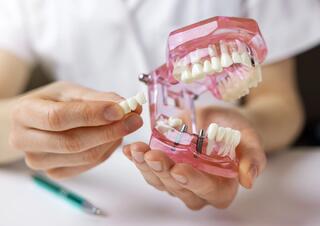
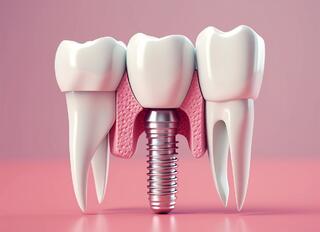
The article on DentalEduc provides a detailed overview of the contraindications for dental implantation, dividing them into absolute and relative categories. We discuss the conditions under which implantation is not possible and when preliminary treatment is required. From diabetes to cardiovascular diseases – we explain how to prepare for implantation and what innovations allow expanding options for patients.
Relative Contraindications for Implants
This category includes limitations that can be overcome. This involves treating diseases or making pharmacological adjustments.
Included are:
- Anemia
- Sinusitis
- Diabetes
- Hepatitis, HIV
- Thyroid issues
- Periodontitis, gingivitis
- Past cancer conditions
- Cardiovascular diseases
- Granulomas, cysts, cavities, plaque
Poor Oral Hygiene
Plaque, cavities, and other issues create an environment for harmful bacteria leading to soft tissue inflammation. To reduce risks, professional cleaning is required.
Managed Diabetes
Previously, diabetes was a barrier due to slow tissue regeneration. Advances in treatment now make tooth row restoration possible for those with controlled glucose levels.
Bone Tissue Atrophy
A lack of teeth leads to a reduction in bone tissue. Bone grafting is necessary before placing implants to ensure success.
If the bone tissue is significantly damaged, increasing its volume isn't always required. Sometimes, a surgeon can place cheekbone implants. They are longer than usual and are inserted into the dense cheekbone. The All-on-4/All-on-6 methods also allow avoiding bone grafting.
Smoking
Smoking slows blood circulation in the gums, and hot smoke damages the oral mucosa. This hinders soft tissue healing and the fusion of the implant with the bone. Doctors recommend quitting smoking at least one month before and after the procedure.
Incorrect bite
Teeth incorrectly positioned next to the implant site can obstruct the surgeon's view during the operation. Therefore, orthodontic treatment to correct anomalies is recommended before proceeding with the implant.
Relative contraindications in women
Pregnancy and breastfeeding
During pregnancy and breastfeeding, the immune system is weakened, which may affect the integration of the implant. Anesthetics can harm the baby. It is advised to undergo implantation no earlier than six months after childbirth.
Menstruation
During menstruation, blood clots more slowly, increasing the risk of bleeding. The implantation is thus performed later.
Relative contraindications in the elderly
Osteoporosis
Osteoporosis makes the bones weak and porous due to a lack of calcium. In such cases, the implant may not achieve primary stabilization. The surgeon may recommend bone grafting or a sinus lift.
Absolute Contraindications
There are scenarios where implantation is not viable. In these instances, the implantologist refers the patient to a prosthodontist to find an alternative method of tooth restoration. Alternatives to implants could include bridge, clasp, or acrylic partials.
The absolute contraindications comprise:
- Hemophilia
- Pregnancy
- Cancer
- Breastfeeding
- Hypertensive crisis
- Rheumatoid arthritis
- Alcohol or drug dependency
- Being underage (below 18)
- Diabetes that is not under control
- Allergy to the materials used in implants
- Mental health disorders that prevent adherence to medical advice
- Having undergone heart surgery or experienced a heart attack in the past 6 months
Decompensated Diabetes
When blood sugar levels cannot be managed with insulin, immunity weakens, leading to abnormalities in blood circulation. These conditions impair regenerative abilities, adversely affecting the success of implant integration.
Autoimmune Diseases
Disruptions in the body's systems may lead to the artificial root being rejected as a foreign object, exacerbation of existing illnesses, and severe deterioration of health. The response of the immune system to such situations is unpredictable.
Blood Clotting Disorders
Preparing the site for the titanium rod necessitates an incision in the gum. Thus, the procedure is impractical if the patient suffers from hemophilia or is required to take medication that thins the blood.
Relative Contraindications – What to Do
There are various diseases considered as relative contraindications for the placement of teeth implants. However, this does not entirely exclude the procedure for the patient. The success of the operation depends on the specific disease and a comprehensive approach by the treating professionals to adjust the patient's health condition.
Diabetes
The chronic disease of the endocrine system leads to an increased blood sugar level, resulting in gum diseases, poor wound healing, and an increased risk of infection complications. Therefore, diabetics were previously not given implants. However, advancements in implantology and endocrinology have made this condition no longer a barrier to a beautiful smile. Scientific studies and the experience of doctors have proven that with proper blood sugar control, implant treatment is successful in 98% of cases. Surgeons apply the classic method of insertion. Initially, an implant with a cap is placed, after 4–6 months a gum former is attached. Two weeks later, impressions are taken, and a crown that properly distributes the chewing force is made.
Cardiovascular Diseases
The surgery is only conducted after a prior consultation with a cardiologist to exclude the risk of aggravating the condition. If the patient is taking anticoagulant medications, their dosage can be reduced or temporarily discontinued with the doctor's permission to prevent postoperative bleeding. During the medical history collection, the implantologist checks whether heart surgeries were performed in the last 6 months or if there were acute cardiovascular diseases, such as bypass surgery or a heart attack. If this information is confirmed, the surgical intervention is postponed to a more favorable time.
Thyroid Diseases
Implantation with thyroid issues is feasible. The decision on the surgery is made together with an endocrinologist. The patient's condition, whether hypothyroidism or hyperthyroidism, must be stable. This is necessary to prevent high blood pressure, emotional instability, and other processes from provoking bleeding or rejection of the implant. Taking prescribed medications is mandatory. Regular checks of thyroid hormone levels and the condition of the jawbone into which the implant is placed are required.
Cancer
Implantation is not performed during cancer treatment. The procedure becomes feasible after completing chemotherapy or radiation therapy, once the individual has fully recovered. It is not possible to specify an exact time since it depends on the radiation dose and the patient's condition. Typically, an oncologist can approve surgical intervention 9 to 12 months later.
Periodontitis, Gingivitis
Gingivitis, a rare disease characterized by the destruction of gums, bone, and ligaments supporting and surrounding the teeth, is not a contraindication. Thus, teeth with mobility are removed, and implants are placed instead. Bone grafting is conducted if necessary.
Periodontitis, an inflammatory disease, is accompanied by gum bleeding during teeth cleaning, pain, exposure, and mobility of teeth, and bad breath. Initially, the infection is eliminated through periodontal cleaning of subgingival deposits, medication is prescribed, and the patient is taught proper oral hygiene. After controlling the inflammation, implants are placed.
Anemia
In most cases, standard dental treatment is ineffective for people with iron-deficiency anemia. Such patients need to identify the cause of anemia, considered a syndrome of some diseases. Medications restoring the optimal iron level in the blood are prescribed, followed by the commencement of implant placement.
Hepatitis B, C, and HIV
Prosthetics on implants for these viral diseases is feasible. Each case is reviewed together with the treating infectious disease doctor. The treatment scheme is selected based on the health status assessed after examination. Test results will clarify for the specialist whether the body can handle the planned operation.
Granulomas, Cysts, Cavities, Dental Tartar
The listed dental diseases are chronic sources of infection that might provoke implant rejection. Therefore, sanitation is conducted before the operation. It includes treating cavities and their complications, gum diseases, removing dental deposits with an ultrasonic, and Airflow powder jet device. In the absence of pathogenic microflora and the toxins they release, the wound heals normally, and the implant integrates into the bone.
Sinusitis
If the implantation is planned for the lower jaw or the upper front teeth, sinusitis is not considered a contraindication. However, its treatment is necessary since any infection reduces immunity. For the restoration of teeth numbers 5, 6, 7, closely located to the sinus floor, an infection is unacceptable as it could lead to the rejection of the implant.
Patients suspected of sinusitis are referred to an ENT doctor. Once the diagnosis is confirmed, the doctor determines the cause of the illness, prescribes medication, or performs surgery. After the inflammatory process in the maxillary sinuses has been eliminated, approximately 1.5–2 months later, the dentist can place the implants.
Specifics of Implantation in Women, Elderly, and Smokers
The implantologist considers not only absolute and relative contraindications. For a successful procedure, the specialist must be aware of certain physiological and pathological changes in the human body. These depend on the patient's gender, age, and existing bad habits.
Dental Implants in Women
The surgeon and the female patient should be aware that there are situations when the operation is postponed to a more favorable period:
Dental Implants During Pregnancy
The placement of implants requires radiological examination, taking antibiotics, and anti-inflammatory drugs, so the procedure is not performed. Additionally, the immune system weakens, and the body of the expectant mother experiences a calcium deficiency, which is used for the fetus's skeleton development. This deficiency can disrupt the osseointegration process, leading to the rejection of the artificial root. Stress, which can cause premature birth, is also a significant factor.
Dental Implants During Breastfeeding
During breastfeeding, just as during pregnancy, women experience a deficiency of vitamins and minerals. Administered anesthetics and consumed antibiotics and anti-inflammatory drugs can enter breast milk and cause an allergy in the baby. For these reasons, it is better to perform implantation when the child has switched to baby food, and the mother's body has recovered. Without a calcium deficiency and other contraindications, the titanium root's integration will be successful.
Dental Implants During Menstruation
During menstruation, hormonal changes occur in the female body, which can provoke or intensify bleeding from the wound. Therefore, it is undesirable to perform tooth extraction or implantation, especially in the first days of heavy discharge.
Dental Implantation for the Elderly
With correct preparation and adherence to the implantation protocol, and in the absence of contraindications, the success of the surgery and subsequent dental prosthesis is assured. At the end of the treatment, patients will have a beautiful smile and be able to enjoy the taste of their favorite foods.
However, it should be considered that nearly all patients over 70 have chronic diseases. Therefore, in planning for the implantation, the surgeon orders tests to determine blood clotting, glucose levels, thyroid hormones, and other important indicators. Patients are also referred for an electrocardiogram. If indicated, consultations with a cardiologist, endocrinologist, neurologist, and other specialists may be required.
Dental Implantation for Smokers
Smoking negatively impacts the success of the treatment, a fact patients with this harmful habit are duly warned about. The healing process is adversely affected due to increased plaque formation, leading to gingivitis, periodontitis, and bone tissue atrophy.
Smoking diminishes blood circulation, and tissues do not receive the necessary amount of oxygen and nutrients. Toxic substances in the smoke suppress the regenerative function of tissues. Hence, doctors advise against smoking before and after the surgery. Ideally, patients should quit smoking or significantly reduce the number of cigarettes in the future.
Risk Factors in Implant Treatment
Several factors can adversely affect the integration of the implant. To eliminate or reduce their impact, the surgeon meticulously collects the patient's medical history and prepares for the implantation.
Risk factors include:
- Smoking;
- Inadequate oral hygiene;
- Inflammatory diseases of teeth and gums;
- Allergies to medications prescribed post-surgery;
- Taking medications that interact with drugs prescribed post-surgery;
- Taking medications that suppress the immune system, affect blood clotting, and influence local and general bone regeneration.
To ensure your implant's longevity, appropriate hygiene must be maintained. In addition to using a toothbrush and toothpaste, it's crucial to use an oral irrigator, dental floss, and interdental brushes daily for cleaning between teeth. Your dentist can recommend the best options and explain how to use them.
What the success of the operation depends on
For a successful implantation, it is important to consult an experienced dentist. Before starting treatment, the doctor conducts diagnostics and creates a detailed treatment plan. This helps to avoid mistakes and the risk of complications. The restored teeth will be attractive, functional, and durable.
Diagnostics
The implantologist assesses the patient's health, his medical history, and current medications. After examining the teeth and mucosa, the doctor examines the data from the computed tomography of the jaws to assess the bone tissue. X-ray helps to determine if there is enough bone for the implants or if a bone graft is needed. If necessary, the doctor prescribes additional tests and consultations. Treating dental diseases before surgery reduces the risk of implant rejection.
Planning
After diagnostics, the doctor creates a treatment plan, selecting the type and number of implants, as well as the materials for prosthetics. The planning phase includes information about the procedure, its duration, and costs.
Choosing the dentist-implantologist and clinic
When choosing a clinic and a doctor, pay attention to the license and certificates. It is also important that there is a guarantee for the services. High-quality equipment, including a computer tomograph, ensures the accuracy of the procedure and prevents complications. It is important to evaluate the cleanliness of the office and the sterility of the instruments. Read reviews about the specialist and the clinic.
Conclusion
We hope this information was useful for you. For details, make an appointment with an implantologist.
Frequently Asked Questions
Is dental implantation possible with gum disease?
Before proceeding with dental implants, it's essential to treat and manage gum disease, or periodontitis. Active gum disease can lead to implant failure due to infection and loss of bone support. A periodontist can assess the severity of gum disease and recommend a treatment plan to eliminate the infection and improve oral health before the implantation surgery.
What if I have undergone radiation therapy?
Radiation therapy to the jaw can diminish bone quality and healing capacity, making dental implant placement more challenging. This is considered a relative contraindication depending on the radiation dose received and the time elapsed since treatment. An interdisciplinary approach involving an oncologist and a dentist is necessary to evaluate the feasibility of implants in each case. Hyperbaric oxygen therapy before and after implant surgery may be recommended in some cases to improve bone healing.
Are heart diseases a contraindication for dental implants?
Some heart conditions, such as uncontrolled high blood pressure, recent heart attacks, or conditions requiring anticoagulants, may pose a risk during dental implant surgery. They are considered relative contraindications, requiring careful assessment and coordination with the patient's cardiologist.