Peri-Implantitis of Dental Implants – Risks and Treatment
Are you sensing pain and discomfort around your dental implant? If so, you might have peri-implantitis. Peri-implantitis is not just inflammation that can lead to the loss of the implant, but rather a real threat to your health. This article will discuss any questions that you might have, provide guidance, and help you extend the lifespan of your implants.
What Peri-Implantitis and What Does it Look Like?

Peri-Implantitis is an inflammation that occurs around dental implants, leading to the deterioration of the bone. Eventually, the bone weakens and can no longer securely hold the implant, making it loose.
Peri-implantitis manifests as a red "funnel" around the implant. An inflammatory area develops between the healthy bone and the mucous membrane. The bone is covered with granulations to prevent the spread of inflammation. The mucous membrane turns red due to poor blood circulation, and the tissues die off.
Initially, the inflammation occurs in the soft gum tissues around the implant. At this stage, known as mucositis, the jawbone is not affected. The primary cause is bacterial growth due to poor oral hygiene.
If mucositis is not treated, the inflammation spreads to the bone. It is crucial to visit a dental clinic as soon as possible to save the implant, especially in the early stages of the disease.
In the initial phase, peri-implantitis often occurs without noticeable symptoms. It can only be detected using X-ray or CT scans, where adjacent tissues are analyzed. Implantologists conduct a series of check-up examinations to monitor the bone healing process.
Symptoms and Signs of Dental Implant Rejection
Identifying signs of peri-implantitis can be challenging as they resemble ordinary inflammation. Common manifestations of this complication include:
- Formation of a periodontal pocket around the implant neck. Separation of tissues from the prosthesis (crown/abutment).
- Pus discharge or bleeding upon touch or during tooth cleaning.
- Increase in body temperature of up to 38º.
- Redness or swelling of the mucosa around the implant.
- Reduction in bone volume, leading to the loosening of the implant.
- Unpleasant mouth odor.
- Pain and discomfort when chewing.
How do we distinguish between peri-implantitis and a temporary inflammation?
It is advised to not delay consulting a dentist. Only a professional can assess the condition of the tissues around the implant and prevent damage to the titanium screw.
Classification
The stages of development are characterized by gradually appearing symptoms. The severity of the condition is determined by the extent of atrophy.
- Normal Condition. No signs of peri-implantitis – no symptoms of inflammation. The X-ray shows the tissues tightly surrounding the implant.
- Early Stage. In the first month, a bacterial biofilm forms around the surface of the implant. The soft tissues become inflamed, disrupting the connection to the bone. Symptoms include mild redness and swelling. Bleeding may occur during examination. The X-ray reveals a slight loss of bone mass (up to 20% of the original level). The implant remains stable. However, without treatment, the inflammation can lead to the degradation of the supporting tissues and the mobility of the implant.
- Moderate Peri-Implantitis. This stage can be noticed by the patient within 3-12 months. The inflammation worsens, leading to the formation of deep gum pockets. Pus may secrete from this area. X-rays show bone atrophy ranging from 20% to 50%. The implant begins to loosen, and the jaw structure changes. Peri-implantitis destroys the tissues around the implant. The patient may experience pain or discomfort while chewing.
- Progressive Peri-Implantitis. Significant vertical atrophy along the implant root is noticeable. Severe inflammation leads to the formation of connective tissue granulations. The implant can break due to its mobility.
Treatment most likely requires surgical intervention. The doctor removes infected tissue and performs bone grafting with mucosal restoration.
We emphasize the importance of early diagnosis and timely treatment of complications. Regular examinations, cleaning, and care of implants are crucial for detecting early signs of peri-implantitis.
What Does Mucositis Have to Do With It?
Mucositis is caused by the accumulation of bacteria on the surface of implant components. This leads to inflammation of the soft tissue. Without treatment, mucositis always progresses to a more severe form of peri-implantitis. This results in the spread of inflammation, increases bone resorption, and makes the implant loose.
Mucositis and peri-implantitis are two phases of the same disease. The difference lies in the severity and irreversible consequences for the jaw. Mucositis primarily affects the soft tissue, while peri-implantitis penetrates deeper into the jaw.
In 43.8% of cases, mucositis develops first, followed by peri-implantitis. It can also be caused by smoking, inadequate oral hygiene, or periodontitis, and then progress to a more serious stage.
Causes of Peri-Implantitis
- Osteolysis of the bone and accumulation of bacterial plaque. After implantation, the bone in the neck area becomes denser, leading to "callus formation." The implant integrates, but a funnel shape forms around it. Poor hygiene leads to the formation of plaque and microbes, causing an infection that can lead to the rejection of the implant.
- Periodontitis. An infection from adjacent teeth can spread to the implant area. Periodontitis increases the activity of osteoclasts, cells that destroy tissue. This results in the formation of a periodontal pocket and the mobility of the implant.
- Smoking. Nicotine reduces blood flow to the bone tissue, impairing wound healing and the body's immune response.
- Incorrect Selection of Implant Parameters and Position. Placing a thin implant in place of a large tooth leads to excessive pressure on the bone. Under strong chewing force, plaque accumulates under the crown, which is difficult to remove.
- Method of Fixing the Crown to the Implant. The use of cement can cause gum inflammation, especially in cases of atrophy in the neck area of the implant.
- Diabetes Mellitus. Affects blood supply and tissue healing. Inflammation often occurs with unstable blood sugar levels.
Diagnosis of Peri-Implantitis in Dentistry
If a patient notices signs of inflammation after implantation or if the doctor detects them during an examination, a diagnosis is carried out.
- Computer Tomography (3D): Helps the doctor determine the cause of the inflammation. Assesses the condition of the bone around the implant and its integration into the bone.
- Panoramic X-ray: Provides a two-dimensional image of the entire jaw. Reveals hidden problems in the jawbone and soft tissues.
- Periapical X-ray: Shows one or two teeth. Displays the crown, the root of the implant, the gum, and the surrounding bone tissue. Helps to identify the location of the inflammation.
- Probing: The doctor evaluates the depth of the gum pockets and the extent of bleeding.
Based on these results, the doctor diagnoses and prescribes treatment.
Treatment of Peri-Implantitis
Important!
Treatment of peri-implantitis is only possible if the implant is immobile. If there is any movement of the implant, its removal is necessary.
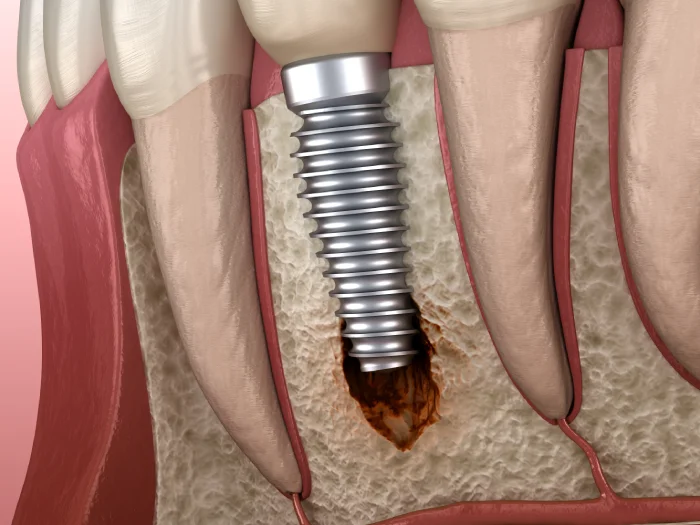
Treatment if the doctor uses conservative methods to treat inflammation, gingivitis, or abscesses around the implant. If bone destruction and granulation occur, surgical intervention is required for cleaning and tissue restoration, as well as for attaching the gum.
Non-Surgical Therapy
- Cleaning the Implant Surface: The dentist performs professional oral hygiene and disinfects the root surface with an antiseptic. He/she cleans the area around the gum with curettage or an ultrasonic scaler and removes granulations, polishing the implant surface.
- Antiseptic Treatment: The dentist treats the area around the implant with an antiseptic (hydrogen peroxide or chlorhexidine solution). He/she applies a gauze pad and treats it with saline solution. A follow-up visit for cleaning and monitoring tissue regeneration is scheduled. The frequency of visits depends on the severity of the complication.
What Medications Can a Doctor Prescribe in Addition to Non-Surgical Therapy?
Antibiotics for Peri-Implantitis: If pathogenic microflora is detected, the doctor may prescribe systemic antibiotic therapy.
- Amoxicillin: A broad-spectrum antibiotic. Taken for up to 14 days (500 mg, 1-2 times daily).
- Metronidazole: Effective against anaerobic bacteria. Recommended dosage is 250-500 mg per day for a week.
A patient's body can be resistant to antibiotics, and the doctor may order a microflora test to select the appropriate medication. Do not take antibiotics without a doctor's prescription and adhere to the prescribed dosage and duration.
What Can Be Used for Mouth Rinsing?
- The dentist may recommend rinsing with a chlorhexidine solution (0.12%) until the next examination. Antiseptics destroy the bacterial film.
- Rinsing Procedure: Clean the teeth with a brush or dental floss. Rinse the mouth with 10-15 ml of the solution for 30 seconds. Rinse all teeth. Spit out the solution, do not swallow.
- It is advised to rinse with chlorhexidine twice daily for 2 weeks.
How Can You Relieve Pain?
The dentist may prescribe a pain reliever (ibuprofen or acetaminophen), especially in cases of acute inflammation or mobility of the implant.
Surgical Treatment
The dentist removes the crowns to access the abutment and connections. The gum under the prosthesis can be severely inflamed, with secretion or pus.
The dentist detaches the gum flap over the implant, and he/she examines the affected bone area. Then, he/she places implant caps or gum formers and removes all bone granulations.
The dentist grinds down the thread and polishes the implant surface. He/she then removes damaged bone areas to stimulate tissue regeneration.
To restore the mucosa, the dentist increases the thickness of the gum contour. He/she connects the tissues with a connective tissue graft or collagen matrix, and tightly sutures the gum flap. He/she provides recommendations for gum recovery (3-4 weeks). The stitches can be removed after 10-14 days.
The dentist installs a gum former, as in standard implantation, and selects new prosthetics (abutments, connectors).
Initially, a temporary crown is fixed. An X-ray of the rehabilitated area is taken, and impressions for the permanent crown are made. After prosthetics, the dentist schedules examinations 3 and 6 months post-treatment.
Re-Implantation After Implant Rejection
The dentist decides on treatment if there is no implant rejection. Removal of the implant and repeat prosthetics may be necessary.
Procedure for Re-Implantation:
- Decision on root removal, bone augmentation.
- Eliminate inflammation, treat gums if necessary.
- Osteoplasty 2-3 months after removal.
- Insertion of new implants 3-4 months after bone regeneration.
- Prosthetics with temporary crowns after complete osseointegration (3-6 months).
Prevention
The dentist decides on treatment if there is no implant rejection. Removal of the implant and repeat prosthetics may be necessary.
Procedure for Re-Implantation:
- Adhere to oral hygiene: regular tooth brushing (twice daily), use of a soft brush and dental floss, professional cleaning by a hygienist.
- Avoid excessive chewing force: limit hard food, consult if you suffer from teeth grinding.
- Balanced diet: limit sweet, sour, and spicy foods to prevent caries and gum inflammation.
- Abstain from smoking and alcohol: reduce the risk of inflammation.
- Regular dental visits: visit the dentist every 3-6 months for monitoring healing and detecting complications.
Q&A
What causes peri-implantitis?
The main causes are poor oral hygiene, infections, smoking, improper care of implants, and associated diseases such as diabetes.
How is peri-implantitis diagnosed?
Diagnosis includes a dental examination, X-ray, or CT scan to assess the condition of the bone and tissues around the implant.
Can peri-implantitis heal on its own?
No, without appropriate treatment, the condition can worsen. It is necessary to consult a specialist.
Does nutrition affect the risk of developing peri-implantitis?
Improper nutrition can contribute to the development of gum and tooth diseases, which indirectly increases the risk of peri-implantitis.
Is peri-implantitis dangerous to health?
Yes, it can lead to the loss of the implant, the spread of infection, and further deterioration of the teeth and gums.
Can peri-implantitis be prevented?
Yes, through regular oral hygiene, quitting smoking, and regular dental visits for preventive check-ups.
Is it possible to install a new implant after peri-implantitis?
It is possible, but this depends on the overall condition of the jawbone and the success of the peri-implantitis treatment.