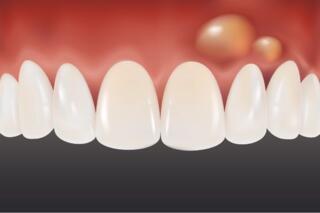
Every morning, standing in front of the mirror, we are confronted with one of the most important aspects of our health and beauty – our smile. But what if this smile isn't as flawless as we would like? Tartar, like an uninvited guest, settles on our teeth. This isn't just a cosmetic issue; it signals hidden threats to our health.
The article you're about to read will not only tell you how to fight this ailment but also unveil many myths and misconceptions associated with tartar removal from teeth.
What Is Dental Tartar?
Dental tartar is a hardened plaque. If soft deposits are not removed daily, they mineralize and harden. These deposits can only be removed by a dentist.
Hard deposits often form in hard-to-clean areas: on the backside of the front teeth and between teeth. They are caused by poor hygiene, insufficient hard food in the diet, and disrupted mineral exchange.
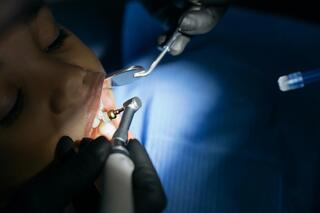
In most cases, deposits are removed with ultrasound. This method gently removes the tartar without damaging the teeth. For gum diseases, tartar is removed by curettage.
Indications and Contraindications
Indications:
- For diagnosing conditions underneath the tartar;
- For prevention or treatment of dental and gum diseases;
- Before whitening, filling, applying braces, or prosthetics.
Contraindications:
- Viral infections, pregnancy, asthma;
- Stomatitis, enamel sensitivity, wearing braces;
- Heart diseases, hepatitis, tuberculosis, HIV;
- Cancerous conditions.
Types of Dental Tartar
Supragingival
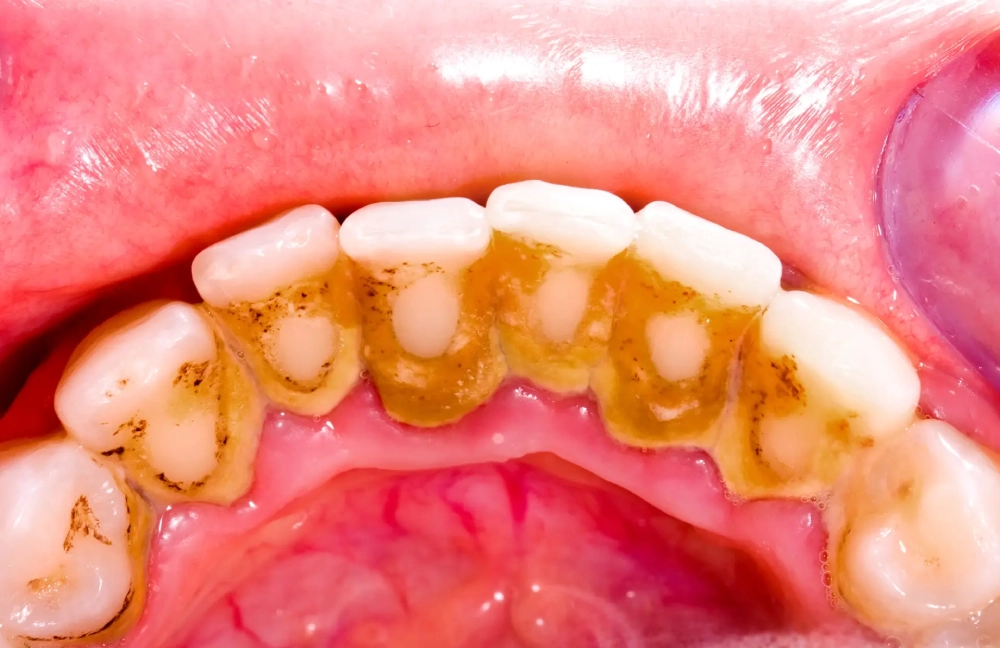
Forms above the gum line, visible to the naked eye. Softer than subgingival tartar. Can be light, yellowish, or dark in color. Caries may develop underneath it.
Subgingival
Hides beneath the gum, covering the tooth root. Detected by the dentist using tools. Indicated by bad breath, itching, blueness, swelling, bleeding. Contributes to gum inflammation and tooth loss.
Tartar Bridge
Forms between neighboring teeth, connecting along the gum line. Occurs if supragingival tartar is not regularly removed.
Supragingival Tartar Removal with Ultrasound
An ultrasonic scaler is used. Ultrasound breaks up and removes the tartar without damaging the enamel. Water or antiseptic is applied during the procedure to clean and cool the surface.
The procedure lasts 30–60 minutes.
Ask your dentist about the cleaning method. Using a metal curette is an outdated method and can harm the tissue, especially in cases of gum inflammation.
Subgingival Tartar Removal – Gum Curettage
Deposits from the subgingival area or periodontal pockets are removed during either an open or closed curettage, depending on the clinical situation: the size of the gingival pockets, the condition of the mucous membrane, the ligament apparatus, and the bone tissue.
1. Closed Curettage
Closed curettage cleans the subgingival area. A modern method involves the use of the ultrasonic device Vector, which works similarly to a scaler for removing supragingival deposits. A thin tip easily penetrates the subgingival area, moving strictly vertically and gently cleaning the neck and root from hard deposits. Simultaneously, an antiseptic, a solution with hydroxyapatite and calcium phosphate, which strengthens the roots and polishes their surface, is applied.
Closed curettage is beneficial for gingivitis, mild periodontitis, and periodontitis. It's used for inflammation around all-ceramic crowns and implants.
2. Open Curettage
Open curettage involves cutting the mucous membrane to clean the neck and roots of the teeth. The dentist can visually assess their condition and perform a thorough cleaning of plaque, tartar, and pathological tissues.
Classic curettage is performed for severe periodontal diseases when the gums recede, teeth become mobile, the size of the periodontal pockets exceeds 4-6 mm, and the alveolar bone is destroyed. During the operation, tooth fixation, bone tissue augmentation, and gum plastic surgery may be performed.
Complications from Dental Tartar
Hard deposits accumulate along the gum line and in periodontal pockets, gradually increasing. They promote the growth of cariogenic bacteria, injure soft tissue, and provoke inflammation.v
Caries
The tooth surface under the tartar can't be cleaned. It is in constant contact with pathogenic microorganisms. The acids they produce leach calcium and phosphorus from the enamel, weakening the tooth's structure and leading to cavity formation. Cervical caries can spread to the root, causing inflammation of the pulp and periodontium.
Gingivitis
Hard deposits trigger gingivitis – inflammation of the superficial gum tissue. The mucous membrane swells, reddens, and may bleed during brushing or biting into hard food, and there may be a periodic unpleasant smell from the mouth. If untreated, gingivitis can progress to a severe form and develop into periodontitis.
Periodontitis
The inflammation affects not only the mucous membrane but also the ligament apparatus holding the tooth, leading to the resorption of soft tissues. Interdental papillae decrease, the gum edge recedes. Periodontal pockets may form and discharge pus. Also, the bone tissue deteriorates: the walls of the sockets holding the tooth roots. As a result, teeth shift, become loose, and can fall out if not timely treated by a dentist.
Use of Anesthesia
Teeth cleaning doesn't cause discomfort because it occurs without direct contact with the tip. However, patients with hypersensitive enamel and exposed tooth necks may experience pain from the ultrasonic effects. In such cases, a numbing gel is applied, making the procedure as comfortable as possible. Before performing open curettage, microinjections of the latest generation anesthetic are administered.
In the first 2-4 days after ultrasonic teeth cleaning, the sensitivity of the enamel increases. During this period, it is recommended to avoid irritants in your diet: cold and hot foods and drinks, hard foods, acidic and spicy dishes.
Examples of tartar removal work
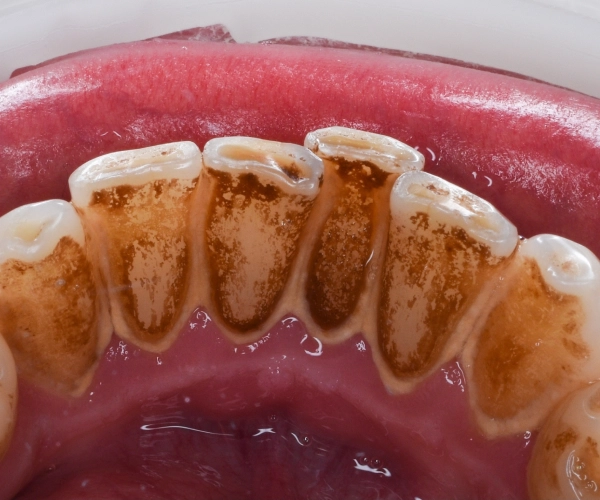
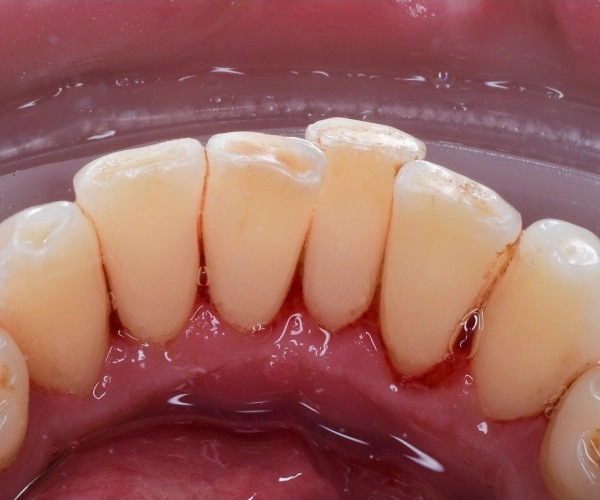
Frequently Asked Questions
What is dental tartar?
Dental tartar is hardened plaque that forms on teeth from food residues, bacteria, and minerals.
Why is it important to remove dental tartar?
Removing tartar is important for preventing gum disease, cavities, and bad breath. Dental tartar can lead to gum diseases such as gingivitis and periodontitis.
How is dental tartar removed?
Dental tartar is removed by a dentist using special tools, such as an ultrasonic scaler.
Can dental tartar be removed at home?
It is difficult to completely remove dental tartar at home; it is better to visit a dentist.
How to prevent the formation of dental tartar?
To prevent tartar, it's important to brush your teeth regularly, use dental floss, and visit the dentist for preventive cleanings.
Is removing dental tartar painful?
The procedure is usually not painful but may cause discomfort. If necessary, the dentist can use local anesthesia.
How long does it take to remove dental tartar?
The time depends on the amount of tartar; the procedure usually lasts from 30 minutes to an hour.
How often should dental tartar be removed?
It is recommended to undergo professional teeth cleaning by a dentist once every 6-12 months.
Does diet affect the formation of dental tartar?
Yes, sugary and starchy foods promote the formation of plaque, which can turn into tartar.