Why Does Tongue Coating Form?
A natural reason is the formation of a light (white/clear) coating during sleep when bacteria in the mouth become active. This coating, through which taste buds are visible, can be easily removed with a toothbrush during regular tooth cleaning. Other cases require special measures. Here are the most common reasons.
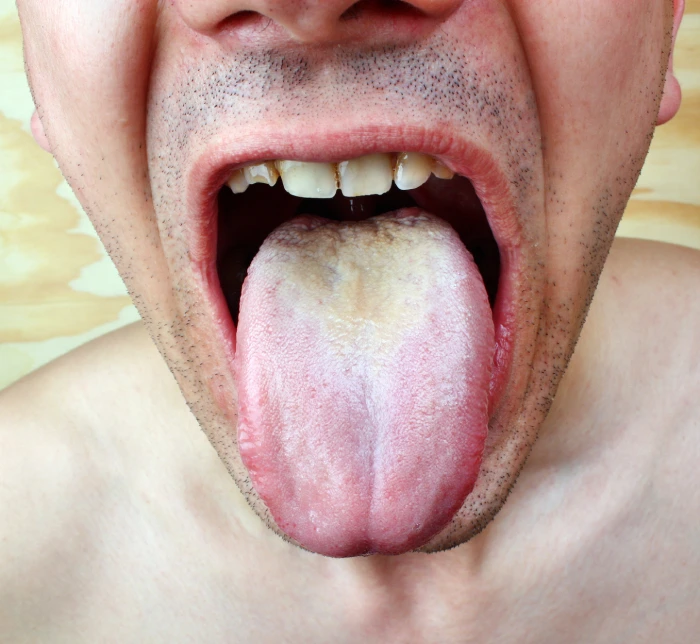
Tongue Coating in Gastritis
Symptoms vary depending on the form of gastritis:
- Chronic: Whitish deposits change to a dark gray coating. They become denser.
- Gastritis with a stomach ulcer: The surface of the tongue turns red, and firm gray coatings appear. Patients complain of burning in the mouth.
- Acute: A sticky white or gray coating forms on the tongue. The mouth feels dry and tastes sour.
Coating on the Tongue in Infectious Diseases
Regardless of the type of infection, the infection weakens the immune system and increases the number of harmful microorganisms in the mouth:
- In Thrush: White, cheese-like deposits form on the tongue. They are dense and cannot be removed with a toothbrush.
- In Diphtheria: The palate arches, root, and back of the tongue are covered with a gray-white layer. Attempting to remove it causes bleeding.
- In Scarlet Fever: Gray-white or yellowish deposits densely cover the tongue. On the 5th-6th day of illness, the coating disappears, the tongue turns bright red, and its surface shows swollen buds.
During and after COVID-19, in addition to a whitish coating on the tongue, there may be sensations of tingling and burning. Small hemorrhages can appear on the tongue.
Tongue Coating in Oral Diseases
When dental plaque accumulates, it can spread to the tongue. Yellow coating often appears on the sides of the tongue. This may be accompanied by inflammation of the oral mucosa – stomatitis or glossitis. Inflammation of the tongue, in addition to white coating, can cause pain due to inflamed taste buds.
Tongue Coating in Respiratory Diseases
In pneumonia and bronchitis, the coating usually appears on the sides of the tongue. It is white and easily removable, but quickly reappears. Symptoms include swelling of the tongue and paleness of the mucous membrane. The taste can become dull, and the mouth feels dry.
Tongue Coating After Antibiotics
A coating can occur due to a disruption in the acid-base balance of the microflora from antibiotics. After starting treatment, the oral environment becomes more alkaline, leading to coating. Cleaning the tongue may cause pain and a sensation of a lump in the throat.
Other Causes of Tongue Coating
The cause can be not only diseases and medications. If the tongue is coated, it could be due to:
- Smoking. Smokers develop a dense yellowish coating due to tar.
- Diet. Consuming soft food or products with dyes can lead to a coating of the corresponding color on the tongue.
- Dehydration. White coating and dry mouth are the result of a lack of water. This is associated with a decrease in saliva production.
The coating at the tip of the tongue is less pronounced than at the base. This is because the tip of the tongue is mobile and often moistened by saliva, while the root of the tongue mainly comes into contact with the palate.
What different kinds and colors of plaque means
| Type/Color of Deposits | What It Means |
|---|---|
| White, dense coating on the tongue and unpleasant mouth odor. |
|
| White deposits on the edges of the back throat wall. |
|
| Pale white surface of the tongue. |
|
| White, curd-like coating on the tongue and inside of the cheeks. |
|
| White-yellow or yellow coating. |
|
| Brown Deposits |
|
| Gray Coating with Cracks on the Mucous Membrane |
|
| Green Deposits with a Rotten Smell |
|
| Black Formations with Ulcers and Bitterness in the Mouth |
|
| Violet Film or Bluish Tint under Whitish Deposits | Heart disorders. |
| Red Deposits |
|
| Blue Coating |
|
Diagnosis
Initially, the doctor examines the mouth. He looks at the color, density, placement, and smell of the coating. The doctor also assesses the patient's complaints about dry mouth and pain after removing the coating, as well as the ability to eat.
After the initial examination, the doctor may order additional diagnostic procedures. These help to identify the cause of the problem. The procedures are conducted in a specific sequence.
| Procedure | Diagnostic Purpose |
|---|---|
| General and biochemical blood tests. | Determining blood sugar and bile pigment levels. Detection of antibodies against syphilis, HIV, hepatitis B, and C. |
| 13C-Urea breath test. | Diagnosing Helicobacter pylori infection. |
| Bacterial culture from the oral cavity. | Analyzing oral flora, checking for viral infections (stomatitis, gingivitis, candidiasis). |
| Ultrasound examination of the abdominal cavity. | Assessing the condition of internal organs: kidneys, liver, pancreas, spleen, gallbladder. |
| Fibrogastroduodenoscopy. | Examining the mucosa of the upper gastrointestinal tract, including biopsy. |
| Stool examination. | Analyzing digestive functions, absorption of enzymes in the intestine, identification of potentially pathogenic viruses, bacteria, and parasites. |
Treatment Methods
Treatment methods depend on the type and cause of the coating. Typically, doctors start with a hygienic oral cleaning. After professional cleaning, regular home oral care is necessary.
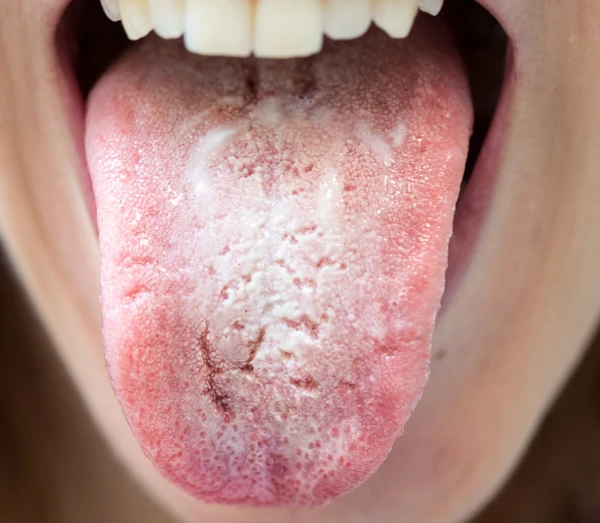
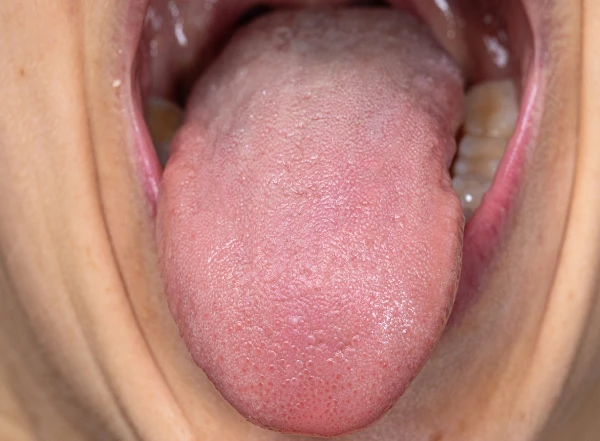
To clean the tongue from deposits, use the back side of a toothbrush or a special tongue scraper. Start at the root of the tongue and gently remove the coating. Finishing the procedure by rinsing the mouth with running water.
- For coatings caused by fungi, antifungal drugs are prescribed in addition to cleaning to restore the gastrointestinal flora. The treatment includes vitamins (B, C, PP) to strengthen the immune system.
- For infectious diseases (tonsillitis, diphtheria, scarlet fever), antiviral medications are prescribed. For bacterial coatings, antibiotic therapy is used. In both cases, treatment is supplemented with antiseptics (e.g., Chlorhexidine, Miramistin).
- Coatings associated with diseases of the digestive tract, kidneys, liver, or respiratory system diminish after treating the underlying disease. The treatment method is chosen individually.
Can the Problem Be Solved Independently?
If a dense coating appears on the tongue that reappears after cleaning, it is essential to consult a doctor immediately. In some cases, the problem can be resolved at home.
| Remedy | Action Algorithm | Effect |
|---|---|---|
| Propolis. | Chew propolis 2-3 times a day. | Strengthens the gums, reduces bleeding, partially removes deposits, disinfects. |
| Herbal infusion. | Steep chamomile and marigold in boiling water, let it infuse. After cooling, strain and rinse your mouth 2-3 times a day. | Strengthens the gums, has an antibacterial effect. |
| Vegetable oil. | Rinse your mouth with 1-2 tablespoons of vegetable oil for 5-7 minutes, then rinse with water. | Absorbs and removes harmful microorganisms from the mouth. |
| Baking soda solution. | Dissolve 3 teaspoons of baking soda in a glass of warm water and rinse your mouth. | Disinfects, softens, and partially removes deposits. |
The information in this section is for informational purposes only. Preventive measures should be used only after consulting with a doctor.
Which Doctor to Consult if the Coating on the Tongue Does Not Disappear?
- Children with persistent coating should be shown to a pediatrician.
- Symptoms of gastrointestinal diseases are a reason to visit a gastroenterologist.
- For signs of a cold, a general practitioner can help.
- If there are no additional symptoms, start with a dentist. If the problem is not related to the oral cavity, the dentist may refer you to a specialist.
Frequently Asked Questions
What is tongue coating?
Tongue coating is a layer of bacteria or other microorganisms that accumulate on the surface of the tongue.
Why does tongue coating occur?
Tongue coating can be a result of poor oral hygiene, certain diseases, smoking, or consuming specific foods and beverages.
Can tongue coating be a sign of illness?
Yes, sometimes tongue coating can indicate infectious diseases, digestive problems, or other medical conditions.
What color of tongue coating is considered normal?
The normal color of the tongue varies from pink to light red, and a slight white coating can also be normal.
When should you see a doctor about tongue coating?
You should consult a doctor if the coating does not go away even after improving oral hygiene, or if it is accompanied by other symptoms such as pain, burning, or swallowing difficulties.
Can diet affect tongue coating?
Yes, certain foods and drinks, especially those high in sugar or colorants, can contribute to the formation of tongue coating.
Does smoking affect tongue coating?
Yes, smoking can intensify the formation of tongue coating and change its color, making it darker.
Can stress cause tongue coating?
Stress does not directly cause tongue coating, but it can indirectly affect the oral cavity, for example, through changes in eating habits or hygiene.