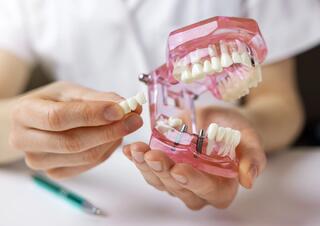
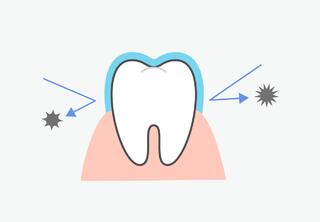
What is a Tooth Nerve?

A tooth consists of a crown, neck, and root. The pulp, located in the crown, is a loosely structured tissue permeated with nerves and small vessels.
The nerve is sensitive to external stimuli and reacts with sharp pain. The basic function of the pulp is to nourish the hard tissues of the crown and tooth root.
Indications for Tooth Nerve Removal
Pulp removal is necessary in the following cases:
- Deep caries leading to infection of the vascular-nerve bundle (pulpitis);
- Presence of a cyst/granuloma with pus at the root apex;
- Inflammation of the tooth nerve as a result of trauma (partially or completely broken root);
- The nerve has decayed/died, and there is an inflammatory process around the root (periodontitis);
- Errors by the doctor (overheating the pulp when preparing the tooth for a crown, perforation of the pulp chamber when removing carious tissues, poor quality root canal filling, etc.);
- Preparing the tooth for a crown placement.
Methods of Removal
Methods of nerve removal are conventionally divided into vital and devital methods.
Vital Methods
The essence of surgical techniques involves extracting part or all of the pulp without its prior death. The operation is performed under local anesthesia.

Vital amputation involves removing the pulp from the initial segment of the root canals (unit cavity and orifices). In the first stage, the doctor removes the nerve, places a therapeutic dressing in the cavity, and sets a temporary filling. After 7-14 days, if there are no signs of inflammation (gum swelling, pain), the dressing is removed, and permanent filling is done. This method is applicable in the treatment of focal pulpitis with well-passable canals.
Vital extirpation involves the complete removal of the nerve (from the pulp chamber and root canals). During the first visit, the dentist completely removes the vascular-nerve bundle, fills the root canals, places a therapeutic dressing, and performs temporary filling. After 7 days, if the patient is not bothered by toothache, the doctor removes the temporary filling material and sets a permanent filling. If the inflammatory process is not pronounced, treatment can be completed in one visit. Vital extirpation is more popular and can be performed even in cases of extensive crown destruction.
Devital Methods
Devital methods involve killing the vascular-nerve bundle with a special compound before extraction. Instead of the former arsenic, modern dentistry uses a non-toxic paste based on paraformaldehyde. The substance is covered with a temporary filling for a week, then the affected tissue is removed, and a permanent filling is placed.
This also involves choosing one of the nerve extraction methods:
- Devital Amputation: The apical fragment of the pulp is removed, while the root portion is treated with a paste to induce necrosis.
- Devital Extirpation: The pulp is initially mummified and then completely removed.
How the Operation is Performed
-
Diagnosis.
The doctor listens to the patient, conducts an examination, collects anamnesis, and directs the patient to X-ray diagnostics.
To assess the state of the nerve, the doctor performs electro odonto diagnosis - applying a small current to the problem unit and observing the pulp's reaction, deciding whether the nerve can be saved.
If necessary, the dentist prescribes CT scans, laboratory tests. Based on the data obtained, the doctor diagnoses and, if appropriate, chooses the method of depulpation. -
Preparation.
After administering local anesthesia, the dentist installs a cofferdam – a special film that prevents saliva penetration and protects the gums from injury. -
Depulpation.
Using a special instrument, the doctor removes the pulp (tooth nerve). It is extracted from the crown part of the problem unit and from the canals. -
Measuring Length.
Using flexible nickel-titanium files (NiTi), the doctor determines the depth of each canal. The quality of the obturation and the minimization of the risk of complications depend on the accurate measurement of their length. -
Expanding the Tooth Canals.
At this stage of treatment, the dentist uses an endodontic tip with pro-files to pass through each canal to the very apex. Removes anatomical constrictions and irregularities. Then expands them in diameter. -
Antiseptic Treatment.
After mechanical cleaning and expansion, they are thoroughly rinsed with an antiseptic solution. -
Filling the Canals.
The doctor fills them with gutta-percha strictly to the very apex. To assess the result, a targeted X-ray is taken. -
Crown Restoration.
Depending on the degree of destruction of the crown part, the doctor places a restorative inlay or strengthens the tooth with a post and core inlay and sets a crown.
Is It Really That Simple?
No. The success of endodontic treatment depends on the dentist's correct performance of the following tasks.
-
Identifying Branches.
Without high-precision diagnostics and experience, the doctor may not identify the presence of additional canals branching off from the main one. If they are not treated with an antiseptic and not filled, an infection will inevitably develop. -
Determining the Length of the Root Canals.
The doctor must fill the canals to the apex of the roots (not lower, not higher). For this, it is necessary to determine the length of each as accurately as possible. If the canal is filled with gutta-percha even slightly below the apex, there is a high risk of developing periodontitis and the formation of a cyst due to the inflammatory process. In the long term, this may even lead to tooth extraction. If the gutta-percha extends slightly above the root apex, the patient may experience pain, neuralgia, numbness of the lip/chin. -
Expanding the Root Canals.
Anatomically, they have constrictions/expansions. If they are not removed with mechanical processing, the doctor will not be able to qualitatively fill the canals with filling material. This will lead to the development of inflammation and ensuing complications.
For mechanical processing, a manual instrument or an endodontic tip is used. The latter gives a result several times better – the surface of the canal walls becomes perfectly smooth (important for filling them with gutta-percha), and the risk of breaking a K-file during immersion is eliminated. -
Filling Method.
It is important to know that filling with paste and a gutta-percha pin almost always leads to complications. In the "Easy Dentistry" clinic, the method of lateral condensation of cold gutta-percha (affordable price, good result) and vertical condensation of hot gutta-percha (the most effective method of filling) is used for filling root canals.
The use of optical equipment – a dental microscope – helps to minimize the risk of postoperative complications. The device allows for the careful removal of all fragments of the affected pulp, preserving the maximum volume of healthy tissues, and guarantees complete sterility of the root canals. The quality of the specialist's work should be checked with a control X-ray.
Post-Procedure Recommendations
After endodontic treatment, patients are advised to follow these guidelines:
- Take pain medication if you experience pain while chewing.
- Remember to take the medications prescribed by your doctor.
- Contact your dentist if the temporary filling falls out (especially when medication is placed for treating periodontitis).
- Do not worry if you experience a temperature increase in the first two days. This is a normal bodily reaction.
If the treated tooth has not been restored with an inlay or crown, do not delay its restoration. After endodontic therapy, the tooth becomes fragile, and there's a high risk of chipping during chewing. If pain intensifies on the 3rd or 4th day, or if swelling increases, inform your doctor.
— For the first 3-4 hours after the procedure, it is recommended not to eat (in extreme cases, you can snack on soft food). Due to the ongoing effect of local anesthesia, you might accidentally injure your tongue, the inside of your cheek, or lips while chewing.
— Completely limit chewing stress on the treated tooth until it is restored with an inlay, permanent filling, or crown.
— Do not apply a hot compress.
How Long Does Tooth Pain Last After Treatment?
After the depulpation procedure, the tooth may hurt for 2-3 days. During this time, you can take pain relievers prescribed by your dentist. If pain persists for a longer period, consult your doctor.
Is Depulpation Painful?
The procedure does not cause pain for the patient. "Live" pulp is removed under local anesthesia. If it is previously killed with a devitalizing material, anesthesia is not needed.
Is Nerve Removal Always Necessary If a Tooth Hurts?
A tooth can hurt even with a perfectly healthy pulp, so depulpation is not always performed. Only a dentist can determine the appropriateness of the procedure in each specific case.
Can a Filling Be Placed Instead of a Crown on a Depulped Tooth?
A depulped tooth can be restored with either a crown or a filling. The choice depends on the extent of the tooth's damage.
What to Do If the Tooth Darkens After Nerve Removal?
For darkened depulped teeth in the smile zone, dentists recommend whitening through canal endodontic bleaching. The procedure involves placing a special whitening compound inside the tooth. The gel's effect results in the lightening of the tooth enamel from within.
Tooth Nerve Removal – What Are the Consequences?
After the procedure, the tooth effectively becomes "dead." This means that the tissues stop being nourished with nutrients and no longer react to external stimuli. The dentin and enamel of the depulped element become fragile. If the technology for cleaning the canals is violated or outdated materials are used during canal filling, the tooth changes color – acquiring a pinkish, bluish, or gray hue.
Here is our case of re-treating a darkened depulped tooth. The tooth lasted 10 years. Our orthopedic dentist prepared the tooth and placed a beautiful zirconia crown with ceramic mass veneering.


Frequently Asked Questions
Is it possible to remove pulp with a laser?
It is currently impossible to perform the operation exclusively with a laser. If necessary, the doctor may use a laser beam for additional antiseptic treatment of the canals. However, the use of a laser does not eliminate the need for mechanical and medicinal treatment of the carious cavity.
Why is pulpitis treatment under a microscope better?
A microscope improves the dentist's visibility, allows for more careful preparation of dental tissues, facilitates work with root canals, and minimizes the risk of medical error.
Can I drink alcohol immediately after treatment?
You should not drink alcohol immediately after treatment. It is necessary to abstain from alcohol for 3-4 days.
Is it possible to avoid surgical treatment of tooth canals?
Yes, if you consult a doctor in time. Patients rarely visit a dental clinic at the first signs of tooth nerve inflammation. Therefore, in most cases, therapeutic endodontics is impossible, and surgical pulp extraction is required.
Book a free consultation with a dental therapist if you have the following symptoms of nerve inflammation:
- Periodic dull or sharp pain in response to thermal irritants, sweet or sour foods;
- Pain while chewing or biting;
- Appearance of gray, yellow, or brown spots (dentin destruction);
- Swollen gums.
And do not delay treating caries, otherwise, bacteria will penetrate to the nerve!
When is root retreatment necessary?
Their repeated revision, cleaning, and hermetic obturation may be required in the following cases:
- Errors were made during initial treatment (non-hermetic filling, inadequate antiseptic treatment, undiscovered canals, root perforation, broken instrument fragment, etc.);
- The crown of the treated unit was not timely restored (bacteria freely penetrated the tooth cavity, causing inflammation);
- The crown fractured due to trauma, infection entered the canals;
- A cyst appeared at the root apex.
Repeated root canal treatment is contraindicated in cases of longitudinal root fracture, critical destruction of the anatomical crown of the problem unit, severe tooth mobility due to periodontitis inflammation, etc.
What symptoms indicate the need for tooth nerve removal?
Symptoms that indicate the need for tooth nerve removal include severe tooth pain, especially when chewing, sensitivity to hot or cold, swelling or redness of the gums around the tooth, and sometimes tooth darkening.
How long do dental implants last?
Dental implants can last many years, often more than 15-20 years, with proper care and regular dental check-ups. Their longevity depends on many factors, including the patient's overall health, oral hygiene, and the quality of the procedure.
Can veneers be placed on damaged or weakened teeth?
Veneers can be placed on damaged or weakened teeth, but restoration may be required first. It is important that the tooth is healthy enough to hold the veneer. In some cases, preliminary treatment, such as filling or a crown, may be necessary.